Treatment Options for Osteoarthritis
There is a good chance that you or a loved one is struggling with osteoarthritis, also known as degenerative joint disease. Osteoarthritis is the most common of all joint diseases, affecting more than 30 million Americans. It occurs when the protective cartilage that cushions the ends of bones wears down over time. Eventually, if the cartilage wears down completely, bone will rub on bone. Ouch! Although, osteoarthritis can damage any joint, the most common sites are the hands, knees, hips and spine. Osteoarthritis symptoms often develop slowly and worsen with time. Symptoms include pain, stiffness, tenderness to touch, loss of flexibility, a grating sensation, bone spurs and swelling.
In this blog, we will discuss the risks associated with a few of the most common treatments prescribed by physicians and what we believe are the safest and most effective options for those with osteoarthritis. If you are struggling with degenerative joint disease, chances are you were prescribed an anti-inflammatory medication (NSAIDS); such as, aspirin, ibuprofen or naproxen. In a 6-year study of 1,700 people with hip and knee arthritis, researchers compared those who regularly took NSAIDS to those who rarely used the medications. The study found that individuals who routinely took NSAIDS had a 240% increase in the development of hip arthritis and a 320% increase in the development of knee arthritis. The researchers are unclear if the NSAIDS are causing a truly negative effect on the cartilage or if the NSAIDS decrease pain and allow people to be more active. Although they are feeling better, when people increase their activity levels they are able to put more load and stress on their joints which can lead to more breakdown of the cartilage and progression of osteoarthritis. Routine use of NSAIDS also increases the risk of GI bleeds, high blood pressure, heart disease, atrial fibrillation and even congestive heart failure. As you can see, for many people the risks of taking NSAIDS may outweigh the benefits. Note: always consult your physician before beginning or discontinuing any medication.
Corticosteroid injections into the arthritic joint are also frequently recommended by physicians. A recent study of 70 people compared the rate of progression of osteoarthritis in patients who received corticosteroid injections to those who didn’t receive injections. The results showed that 44% of patients who received a corticosteroid shot had accelerated progression of osteoarthritis compared to a progression of the disease in only 24% of individuals who did not receive an injection. There is some evidence that corticosteroid injections, especially combined with an anesthetic, can be toxic to cartilage.
You are probably thinking, none of those seem like good options! What am I supposed to do? At Advanced Healthcare and Sports Injury we believe the safer approach would be regular exercise, simple dietary changes and manual therapies such as dry needling. Using these interventions as the pillars of managing these conditions and utilizing medications/injections if there is a severe need or lack of progress would likely be a great strategy. Typically the priority is meds first, then diet, lifestyle and physical interventions last. A study looking at the effectiveness of exercise and diet in the treatment of osteoarthritis in overweight, elderly individuals found that 90% of participants who were dieting and/or exercising reported significant reductions in pain along with weight loss. Those completing both a diet and exercise plan had less pain, better function, faster walking speed and a better self-reported quality of life. The bottom line with all of these studies is that the most effective way to manage osteoarthritis may not be with medications, but with diet, exercise and manual therapies.
A contributing factor to the pain associated with osteoarthritis in many individuals is trigger points or what you may call “knots” in the muscles around the arthritic joint. Research studies show that patients with knee osteoarthritis have more active trigger points than healthy individuals. So what can we do about these trigger points? Dry needling is a treatment that involves placing very thin, solid needles into tight or painful muscles. It is particularly helpful in treating trigger points and stimulating proper muscle function. Research indicates dry needling on active trigger points improves pain and physical function for people with knee and hip osteoarthritis. In other words, treating the painful tissues around the arthritic joint can decrease pain and improve mobility in the arthritic joint(s).
Contact us to let Advanced Healthcare and Sport Injury help you develop a safe and effective treatment plan for managing your osteoarthritis!
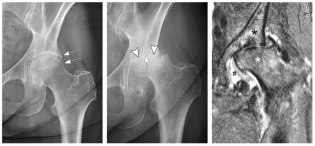
Fig. 1. Rapid progression of osteoarthritis in a 38-year-old female following intra-articular corticosteroid injection.
*images and study references courtesy of Dr. Tom Michaud and humanlocomotion.com
